Open-Label Clinical Trials – How Are They Run and When Are They Appropriate?

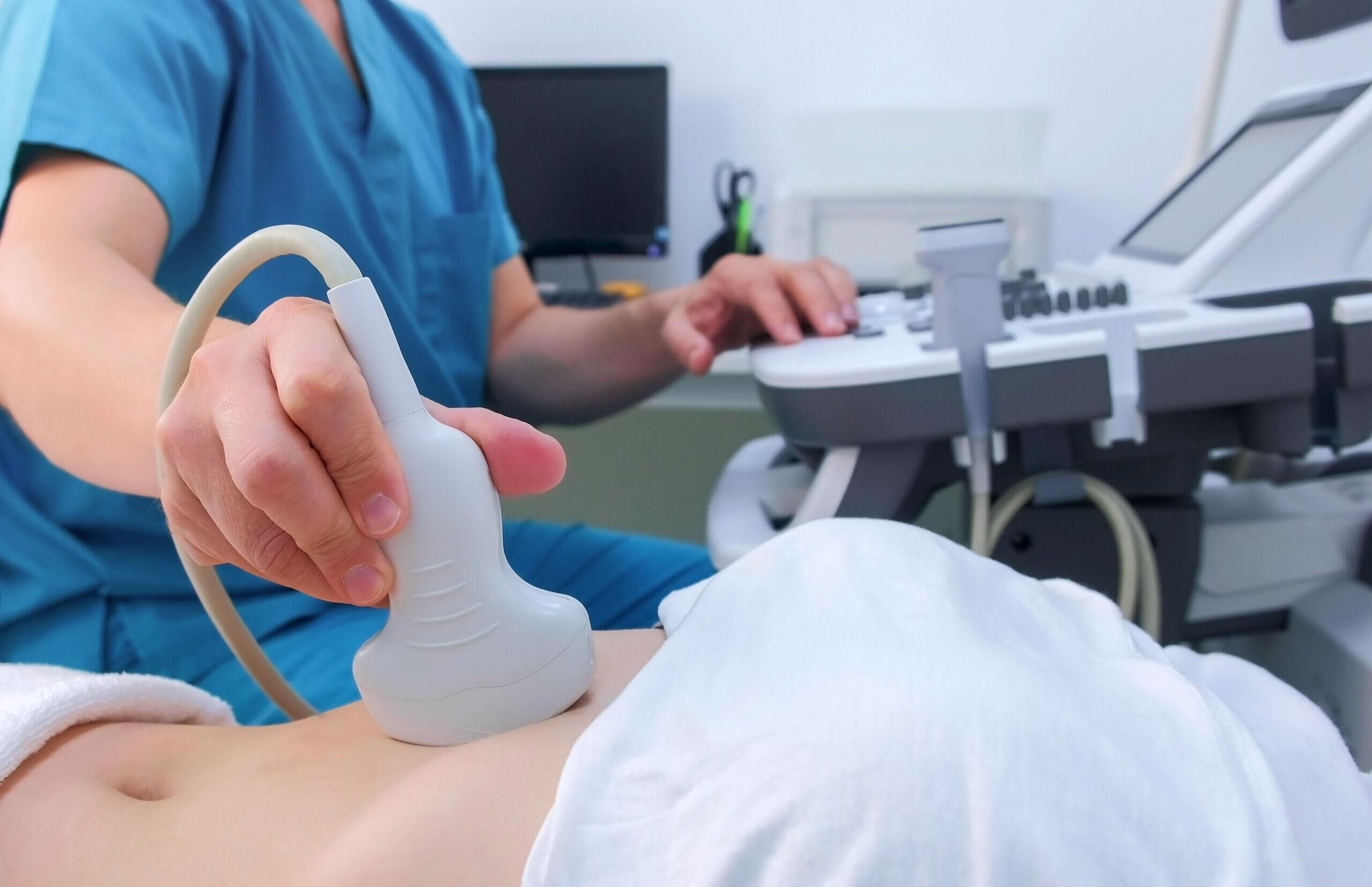
Clinical trials are an integral part of advancing medical treatments, identifying new drugs or therapies, and improving patient outcomes. If and when the testing of new treatments shows success and promise in animal models, will human-based clinical trials be suggested for further testing and evaluation. To ensure patient safety and the reliability of the results, clinical trials must be conducted under controlled, specific, and well-designed criteria. If the clinical trial design is inadequate, this can delay bringing new treatments to market, and even lead to bad conclusions about safety and efficacy of treatments. With this said, let’s take a look at open-label clinical trials, and how and when they are used.
How To Identify An Open-Label Clinical Trial: Modifying Characteristics & Masking Level
The easiest way to identify whether a clinical trial is open-label or not is to look to see if modifying characteristics are allowed (or not), and if there are any masking levels associated with the trial. To make this clear:
1. A clinical trial is open-label if the characteristics of the trial can be amended to solve unexpected events that occur. This is common in clinical trials in Phase I and II, but making amendments along the way can result in less conclusive results. A clinical trial is closed if the initial characteristics of the protocols cannot be changed.
2. An open-label clinical trial can also be identified by the level of masking involved (anonymity). If the patient knows that he/she is being assigned an experimental treatment, what that treatment is, and the investigators are also aware, then this is an open trial. But we’ll get more into open-label clinical trials versus blind studies down below.
The Difference In How Blind Trials vs. Open-Label Clinical Trials Are Run
Understanding the difference between how blind trials vs. how open-label clinical trials are run is important, as the design of the trial can affect the results.
- Blind clinical trials are the most common and involve single-blind or double-blind approaches. A single-blind approach means that only one party (usually the patient) does not know what treatments he/she is receiving – either the control or experimental drug. Double-blind, on the other hand, means that both parties (the patient and investigator) do not know which treatment a patient is receiving. Blind trials are fully randomized, and controlled in the hope of reducing potential bias from either party.
- Open-Label Clinical Trials are different from blind trials in that they contain no “masking” or “blinding” and both parties (the patient and investigator) know which treatment group the patient is in and which treatments are assigned to them. Open-label clinical trials are more commonly used in early phases of testing, as they offer greater flexibility to adapt the protocols along the way, and are used to compare different treatments or to gather additional safety and efficacy information on long-term effects of treatments on the market. An open-label clinical trial may also be called “non-masked” or “unblinded”.
When Is An Open-Label Clinical Trial Appropriate?
When looking at the circumstances in which open-label trials may be appropriate, we need to consider the risks and benefits. Open-label clinical trials are appropriate when randomization of treatments may be difficult, or if it’s important to test long-term effects or safety profiles. They are also used to boost the confidence of clinicians, patients, and clinical bodies about the effectiveness of a treatment that’s already been approved by the regulatory authorities.
It is also appropriate to use an open-label clinical trial in a Phase I or II studies where the incidence of adverse effects have already been identified through a blinded study or pre-clinical study, but the perception of those reactions need to be refined with more data on a given subject or disease.
They may also be useful where there is no control group, like in observational studies where the primary purpose is to examine the progress of a disease in a given population, or in a Phase III Pivotal Trial where there is already a lot of evidence that the experimental treatment works, but more data is needed. Open-label studies are also important for rare diseases, where it may be difficult to find an adequate number of control subjects.
Open-Label Clinical Trials Are Valuable, But Limited
Open-label clinical trials are a valuable tool in the assessment of treatments, particularly when control group randomization is not feasible. They can also provide information on safety profiles, long-term effects, and the efficacy of treatments, while increasing confidence among clinicians about previously approved treatments. That said, open-label clinical trials do have certain limitations, such as being more vulnerable to patient bias and placebo effects due to the lack of blinding for both patients and investigators.
Here at Conquest Research, we conduct clinical research studies to discover better treatment options for patients of today, and the future generations of tomorrow. If you’d like to learn more about participating in open-label clinical trials, or if you have questions about their design, don’t hesitate to reach out and contact us here at Conquest Research.
Sign Up For A Study
CURRENT STUDIES
Conquest Research is continuously looking for participants to take part in clinical research trials for various medical conditions.